L’intossicazione da funghi: come prevenirla e come intervenire
I funghi possono essere velenosi!
A volte anche un raccoglitore esperto può essere tratto in inganno, e anzichè funghi commestibili e innocui finiscono in tavola specie velenose.
Nel racconto “Funghi in città” di Italo Calvino i protagonisti dell’inattesa raccolta domenicale finiscono tutti quanti in ospedale e il racconto termina con una lavanda gastrica collettiva, per fortuna senza gravi conseguenze.
Purtroppo però non sempre l’esito di una intossicazione da funghi è così favorevole come nel racconto!
I dati sulle intossicazioni da funghi: epidemiologia
Pensate che in Italia negli ultimi 20 anni, nonostante le campagne informative, vi sono state centinaia di intossicazioni da funghi. Per evitare di annoiarvi con numeri e statistiche diciamo soltanto che, se si considera l’intero territorio nazionale, i numeri sono davvero importanti, con 13.884 richieste di consulenza al Centro Antiveleni di Milano dal 1995 al 2011, durante i quali si sono verificati 37 decessi e in 15 casi si è dovuto ricorrere al trapianto di fegato (1).
Conoscere i funghi per prevenire le intossicazioni
Per evitare di correre questo rischio se non sei un esperto ma non vuoi privarti del piacere di una passeggiata nel bosco in cerca di funghi, una volta raccolti falli esaminare dal sevizio micologico della tua ASL, il servizio è gratuito! Scopri nel link qui sotto di che cosa si tratta!
L’intossicazione da funghi: i sintomi
Causa dell’intossicazione da funghi: eziologia
Il motivo per cui i funghi possono dare un’intossicazione sta nella presenza di tossine velenose. Le tossine sono delle sostanze tossiche per le cellule del nostro organismo che possono colpire in modo specifico alcune cellule piuttosto che altre. Alcune sono dirette contro l’apparato digerente, altre specificamente contro quello nervoso, eccetera. A seconda del tipo di tossina dipende il tipo di disturbi che si possono scatenare.
L’entità dei disturbi dipende dal tipo, dalla dose e dalla potenza letale della tossina del fungo, che a sua volta dipendono da tanti fattori: in primo luogo dal tipo di fungo consumato (e quindi dal tipo di tossina ingerita), poi occorre considerare l’area geografica di provenienza, la stagione, il metodo di preparazione, la quantità di tossina ingerita e la risposta individuale a quest’ultima (2).
Sintomi più frequenti e comuni dell’intossicazione da funghi
Generalmente la tossina ingerita raggiunge per prima cosa l’apparato gastrointestinale dove determina un danno di gravità variabile, generando i classici sintomi di un’intossicazione gastrointestinale, come vomito, dolori addominali e diarrea: questi in genere si presentano abbastanza rapidamente dopo l’ingestione dei funghi velenosi, da 30 minuti a 6 ore. Normalmente si risolvono entro 24 ore e sono a basso rischio per la vita. In casi più rari i sintomi invece possono comparire dopo 6-20 ore e possono mimare sia una banale gastroenterite che un’influenza, con rischio di sottovalutare i sintomi e ritardare la diagnosi e ritardare così le cure!
Sintomi più rari e pericolosi dell’intossicazione da funghi
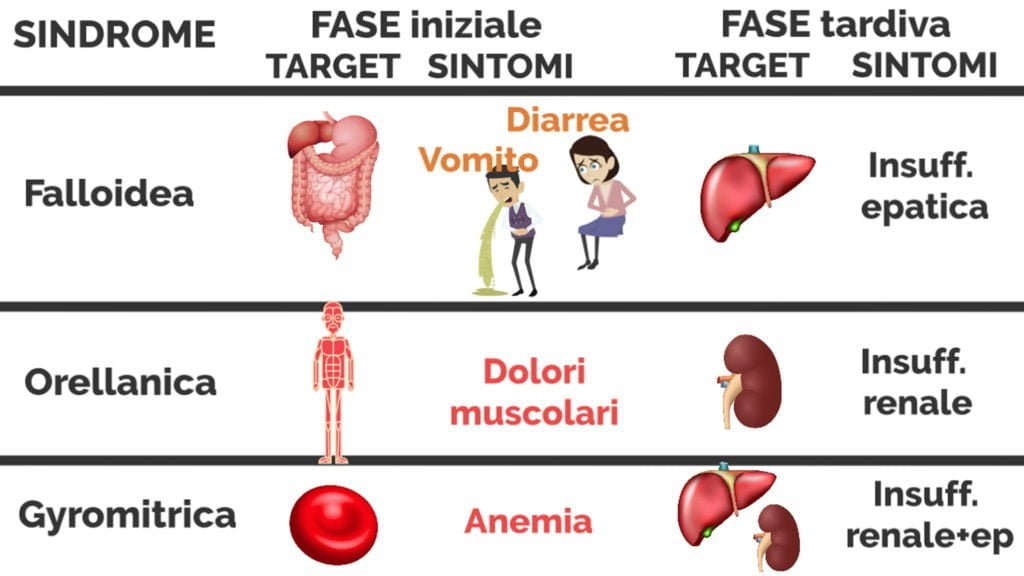
-la sindrome falloidea è caratterizzata da vomito e diarrea ripetuti che portano rapidamente ad un grave stato di disidratazione; superata la prima fase di disturbi gastrointestinali vi è una seconda fase che prevede la degenerazione progressiva del fegato che viene colpito severamente dalla tossina
-la sindrome orellanica determina dolori muscolari (qualche volta associati alla comparsa di rossore cutaneo), mal di testa, riduzione della quantità di urina prodotta, brividi e inappetenza. Questa sindrome può rapidamente evolvere verso l’insufficienza renale.
– la sindrome gyromitrica determina sonnolenza e dolori muscolari ed evolve verso un’anemia emolitica (una forma di anemia dove i globuli rossi vengono distrutti) con danni al fegato e ai reni (3).
Diagnosi e trattamento dell’intossicazione da funghi
Una diagnosi rapida e un trattamento tempestivo portano ad un aumento delle probabilità di sopravvivenza. Per questo motivo chiunque abbia il sospetto di un’intossicazione da funghi deve rivolgersi il più velocemente possibile al più vicino pronto soccorso portando con sé i funghi consumati, sia cotti che crudi. Questo perchè al pronto soccorso viene chiamato anche un esperto micologo in grado di identificare esattamente le specie consumate. Con queste informazioni viene contattato il centro antiveleni che provvede a suggerire la terapia più adeguata per ciascuna forma di intossicazione.
Non esistono antidoti specifici per le tossine fungine responsabili dell’intossicazione, perciò il trattamento sarà finalizzato soltanto a neutralizzare i danni prodotti dalla tossina nei vari organi ed apparati dell’organismo, riducendo le complicanze con l’utilizzo (variabile a seconda dei casi) di farmaci contro il vomito, con proprietà di assorbimento delle tossine o che contrastino gli effetti paralizzanti sui nervi o sulla muscolatura (antiemetici, adsorbenti, anticolinergici o anticonvulsivanti) (4).
Quali sono le reali conseguenze a lungo termine dell’intossicazione da funghi?
La prognosi dipende in larga misura dalle caratteristiche individuali della persona che ne viene colpita, a maggior rischio sono i bimbi e le persone anziane. Una diagnosi rapida e un trattamento tempestivo possono portare ad un aumento delle probabilità di sopravvivenza. Quando vengono colpiti degli organi, come nel caso del rene per i funghi che determinano la sindrome orellanica, anche dopo la guarigione dall’evento acuto ci possono essere danni a lungo termine. Anche in questa circostanza la tempestività dei trattamenti gioca un ruolo fondamentale per la riduzione delle conseguenze a lungo termine.

Bibliografia
(1) Dati del Centro Antiveleni di Milano
(2) Diaz JH. Evolving global epidemiology, syndromic classification, general management, and prevention of unknown mushroom poisonings. Crit Care Med. 2005 Feb. 33(2):419-26.
(3) Ministero della Salute; I funghi, guida alla prevenzione delle intossicazioni
(4) Enjalbert F, Rapior S, Nouguier-Soulé J, Guillon S, Amouroux N, Cabot C. Treatment of amatoxin poisoning: 20-year retrospective analysis. J Toxicol Clin Toxicol. 2002. 40(6):715-57.
Altri articoli utili:
Epis S, Matinato C, Gentili G, Varotto F, Bandi C, Sassera D. Molecular detection of poisonous mushrooms in different matrices. Mycologia. 2010 May-Jun;102(3):747-54
Cervellin G, Comelli I, Rastelli G, Sanchis-Gomar F, Negri F, De Luca C, Lippi G. Epidemiology and clinics of mushroom poisoning in Northern Italy: A 21-year retrospective analysis. Hum Exp Toxicol. 2018 Jul;37(7):697-703